DIALYSIS ACCESS CATHERIZATION
Renal Failure Related Interventions
Access for dialysis – Temporary or tunnelled catheter insertions done under USG and fluoro-guidance for dialysis which are options for emergency or pre-fistula dialysis.

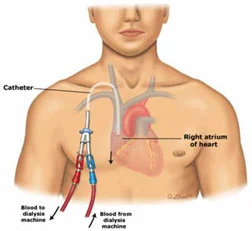
USG and fluoro-guidance makes procedure minimally invasive avoiding multiple punctures and complications which occur due to blind technique can be significantly reduced. USG and fluoro-guidance particularly helps when patient has deranged coagulation profile and platelet dysfunction which is common in chronic kidney disease patients.
Fistulo-plasty – A fistuloplasty is a way of relieving a blockage in the arteriovenous fistula. This allows access for dialysis without having an operation. The blockage is opened up using a special device or ‘balloon’ therefore allowing more blood to flow through the fistula.
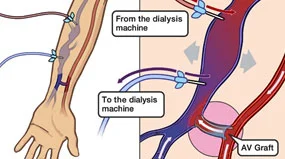

Over time, a fistula can age, and problems such as scarring or clots can decrease its function and the effectiveness of dialysis. Clots can cause blood to flow at a slower rate than the rate your doctor ordered, or block a fistula completely. It is important to restore the recommended blood flow rate and treat clots that are forming at an early stage so that your fistula continues to work well and you get the amount of dialysis you need. If narrowing or blockage is left untreated, it may lead to your fistula failing.
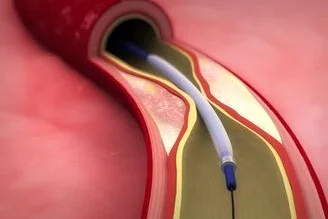
The main alternative to fistuloplasty is surgery to form a new fistula. However, as a fistula is often a preferred dialysis access route, it is worth preserving it as long as possible before creating a new one. It is especially important in patients on long-term dialysis because there are limited blood vessels in the body that are suitable to form fistulas.
Renal Failure Related Interventions
What is central venous occlusion. Venography demonstrating more than 50% stenosis of the subclavian, brachiocephalic vein, and superior vena cava in the upper extremity or the iliac vein or inferior vena cava in the lower extremity is considered central venous occlusion.
Central venous stenosis (CVS) is encountered frequently among hemodialysis patients. Prior ipsilateral central venous catheterization and cardiac rhythm device insertions are common risk factors, but CVS can also occur in the absence of this history. Chronic CVS can cause thrombosis with partial or complete occlusion of the central vein at the site of stenosis. CVS is frequently asymptomatic and identified as an incidental finding during imaging studies. Symptomatic CVS presents most commonly as an upper extremity edema ipsilateral to the CVS.

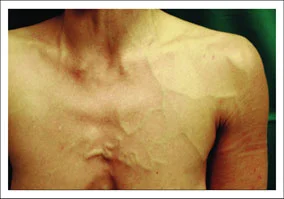
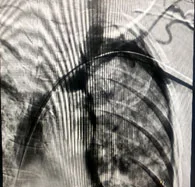
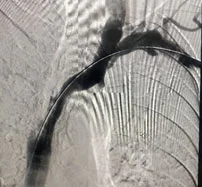
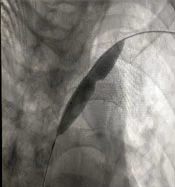
Venous angiography is the gold standard for diagnosis. Percutaneous transluminal angioplasty and stent placement can improve the stenosis and alleviate symptoms, but CVS typically recurs frequently, requiring repeated interventions. Refractory symptomatic CVS may require ligation of the ipsilateral vascular access. Because no available treatment option is curative, the goal should be to prevent CVS by minimizing catheters and central vein instrumentation in patients with chronic kidney disease and dialysis patients.

Book Appointment
-
Varicose Veins & Varicose Ulcer Treatment
-
Non-Healing Wound Management
-
Vascular Malformations
-
Uterine Fibroid or Prostate Embolization
-
Cancer Treatments – TACE, RFA, Embolization
-
Dialysis Access Catherization
-
Diagnostic Procedures – FNAC, Biopsy, Diagnostic Angiography
-
Abscess Treatment - Aspiration, Pigtail Drainage
-
Treatment of Aneurysm and Stroke
-
Deep vein thrombosis (DVT)
-
Other USG, CT & DSA Guided Interventions
